I’m writing the first draft of this blog post at 1:46 AM. The patient I’ve been monitoring since around 10PM has been in active labor for what feels like an eternity. Both the mom and I had such high hopes that the baby would be born before the clock strikes midnight –there was even a little competition between my patient and the patient next door. But babies choose when they want to come out.
I am fairly certain I’m the last intern left in The Medical City.
It’s important to note two things: (1) our shift officially ended 11PM, and (2) I don’t actually have plans to be an obstetrician. But a part of me knows that, after this rotation, I’ll likely never assist in another delivery until I do outside rotations during residency (our patient is almost fully dilated –please don’t convert this NSD into another stat CS!).
And as a future GP or family physician, I need a little more than the handful of babies I caught back in clerkship in Quirino. The rust of year-long online learning has overlain all my previous experience and confidence. What if a pregnant patient goes into labor in an elevator, or an airplane, or right there at the side of the street? I can’t hesitate.
And so I stay.
Read: New doctor’s baptism of fire: Emergency delivery at the backseat of a car
But this all comes at the end of all things. Here’s what happened over the rest of my two weeks in OBGYN first.
Back in the OR complex
My first few weeks in the hospital were spent in the medical floors and in the community. We had no exposure to any surgical field, except perhaps the bedside procedures in the intensive care unit. The potential of removing sutures in a family clinic. Maybe doing rounds on co-managed post-operative patients.
Being back in the operating room came with familiar anxieties. How do you scrub in again? What if I make the field unsterile? What if they ask me questions on anatomy that I can’t answer? WHY IS IT TAKING ME SO LONG TO DO CLOSED-GLOVING???
But the first few days in the LR/DR/OR complex (respectively: labor room, delivery room, and operating room) eased me in. Most of the time, we were only monitoring patients in the IMU (Intensive Maternal Unit). Many of our patients in the first week were mothers carrying twins, who happened to have preeclapmsia or who were going through preterm labor.

.
That first week was when I found out that hours can pass really quickly if you divide it into 15-minute increments –for non-medical professionals, this is because we monitor fetal heart tones every 15 minutes, and vital signs every hour in the IMU. It’s like the pomodoro technique, except the actual work is shorter than the break.
In fact, for the first four duties, we only saw two patients in labor. That’s only two cesarean section procedures in 36 hours. Where did the mommies go?
My first (and only) assist over the first week of my OB rotation was a cesarean section. And even then, I had to push it –she was brought to the OR at 11PM, so I went home around two in the morning. Way past our time in duty.
(Somehow, I’m beating my own record tonight!)
Second week: OB floors, pre-LR, and more
My second week in obstetrics involved more patient interviews and paperwork. However, the experience was still tamer compared to my experience during clerkship –imagine, our floors census one morning was only four pages long! I feel like that’s almost unnaturally short…
Aside from going on two duties in the floors (for a total of 16 hours only, which is still wild to think about), I also spent two duties in the pre-labor room (which functions as a type of ’emergency room’ for OBGYN patients) and one day in the Women’s Health Care Center.
My duty partner for majority of my duties was Kevo (a fairly reliable friend and a great conversationalist) plus or minus a group of clerks rotating only a few hours at a time. I think a highlight of our duty-partnership was a night spent in the pre-LR barely with only a couple of patients and many hours spent talking about politics, philosophy, even religion. (Featuring Doc Bree).
.
Spending a day in WHCC was a whole experience in itself. I honestly regret only having one 8AM-5PM duty in the center; the fellows and consultants were so kind and willing to teach, and there was a neverending flux of patients to sonographically examine.

.
Thank you to Dr. Diaz and Dr. Ursua for taking the time to teach, especially Dr. Ursua for allowing me to use the new ultrasound machine on my own. It was so fun playing around with the 3D settings and light filters, and also chatting with the patient while Dr. went out to take a call. And an equally sincere shout of appreciation to the WHCC fellows, Dr. SDC and Dr. LCA, for their patience with this clueless intern. There’s a learning curve, and that’s fine!
And finally: I even volunteered to help put makeup on some of the OBGYN residents as they prepared for PENTAMED, a type of interhospital competition (I think). Here’s to new experiences and taking initiative!

.
All of these experiences proved to be the best teacher. Even though I can count on one hand the number of times I cracked open Williams (the standard textbook for OB) over the last two weeks, I still got a good score during our end of rotation exam. Ideas and theoretial information really stick when there’s application!
Investing in the future
Our AM-PM schedule comes with a day off per cycle. This ‘day off’ is spent either in telemedicine, simulation lab, or the laundry shop. (I’m getting real familiar with the laundromat downstairs).
The simulation lab was an interesting and fun experience. We finally saw a tiny bit of what the school administration promised at the very start of online/blended learning –fancy machines and models designed to emulate actual patient encounters and clinical exposure.
Meet Hana, a perinatal patient care simulator bought all the way from Japan. ASMPH now owns two of them. Each model (which costs at least half a million pesos, if my googling is in any way accurate) comes with interchangeable modules to check ultrasound, listen to fetal heart tones, do internal examination, simulate normal spontaneous delivery, and so on. There are accessories for intubation and urinary catheterization. There’s even a spot where you can do an IV insertion.

.
Hana even comes with an ultrasound! And it was scarily accurate compared to the real thing in WHCC (see above).
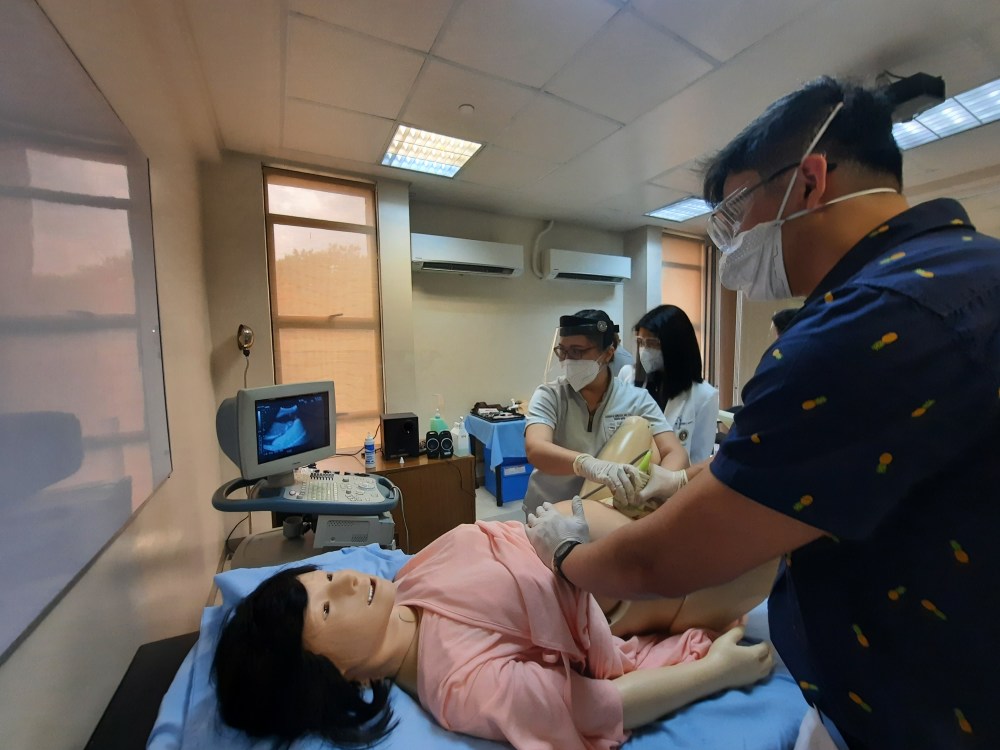
.
Having this uncanny model is a great stepping stone for third and fourth year clinical students. I imagine I would have felt less anxiety interacting with actual patients had I experienced this kind of simulation beforehand. It would also help us understand the “diagnosis and management” section of textbooks better.
For fifth year or post-graduate trainees, the model still pales in comparison to the real thing.
Speaking of the real thing: I am still writing this draft at 2:24 AM. The patient is still “almost fully” dilated. I would like to proceed, please. Hana wouldn’t do this to me.
(But if I aim to do residency here in the Philippines, specifically in a public training hospital, I need a lot more stamina than just facing an end-of-rotation exam, online mass, and eight hours plus-plus of duty).
The inbetweens of internship
First of all, if you haven’t heard –I’m finally fully vaccinated. I can soon stay in with other people. (Who cares about going out).
.
Read: I got the vaccine.
Second: welcome to The Lounge for TMC staff. It’s fairly new, at least to me. I don’t really know what else to say about it, except that this place is pretty. It’s a picturesque and safe (if too warm) place to have a solo meal and chill.

.
And just this Sunday, we’re officially “eagles”! As quoted from the official FB page, Pugad Agila is the Ateneo School of Medicine and Public Health’s medical board exam community-wide operations. As the board takers this coming September 2021, our batch is the focus of attention for this season. We’ve been assigned mentors and ‘tandangs’ (underclassmen who hype us up/help us keep discipline), given study kits, theoretically offered free food…
The program officially launched with mass and a program I only half-listened to, but the effort and anticipation have been building for quite awhile!

.
I even got in touch with both my mentor and my tandang already (my tandang is Jesha, one of the more blog-elusive loves of my life).
But that is definitely for the future.
This, here, now. In this inbetween, I’ve learned that it’s not only absence that makes the heart grow fonder, but also the threat of it. The last two weeks of OBGYN felt so short that I was already missing the experience even as I lived it.
I used to be ambivalent about having to assist in vaginal deliveries and cesarean sections back in clerkship; now I felt frustrated at the lack of opportunity. I didn’t want to volunteer for procedures in the pre-pandemic era; now I want to stitch everything I can and do whatever is humanly possible.
(I hope I’ll feel the same way about surgery).
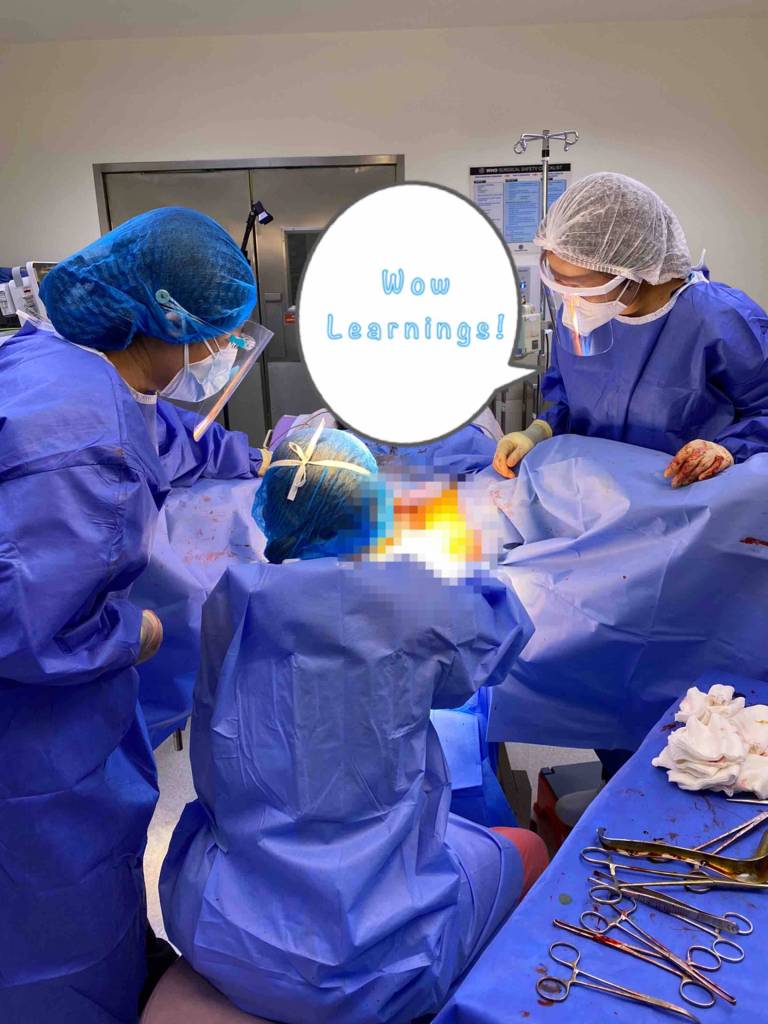
Now it’s well past the witching hour. My patient’s baby has been safely delivered (not via CS, thankfully!). I got the opportunity to assist Dr. Chua (the consultant) and Dr. Chua (the resident). The more senior residents, Chief Dr. Lexa and Dr. Ayra, were coaching the patient (and me!) along. Our consultant was so generous as to narrate and teach, and I even got to see outlet forceps extraction and cord blood collection all in hour. I got to see my patient say hello to her baby.
I’m kinda really sad to see the OB rotation go.
(REALLY FINALLY EXCITED FOR PEDIATRICS THOUGH).
Final thank you to all our lovely OB consultants, residents, nurses, orderlies, and staff ♥️
Until next time!

Say something back.