In the interim | idiom | : at or during the same time : meanwhile
There are words and phrases that can go unheard and unused your entire life. Before I stepped into medical school, “in the interim” was firmly outside my vernacular. Meanwhile. The meantime. Temporary. In between. Provisional.
Then medical school happened, and suddenly every week featured case presentations built on temporal profiles and histories. In the interim, followed by “the patient tolerated symptoms”, or “no medications were taken”, or “mass gradually and painlessly enlarged with no consult done”, or.
You get the point.
This post is for the spaces in between.
From internal medicine to the next
Out of the big four specialties, internal medicine is my favorite. I will die on this hill, though I might take it back when I finally rotate in pediatrics. No clue if or when that will happen. Now that interns and clerks have once again been pulled out of face-to-face rotations (due to an ongoing surge in cases nationwide), I can only look back in gratitude at the fact that, at least, I was able to rotate in IM.
There were many highlights to our rotation in the hospital. First was the ability to see patients again, and to follow their course daily. This privilege to learn from our patients and to see them from one state of wellness to another was something I wrote about in my first blog after onsite internship resumed.
Read here: In the business of saving lives.
The next best thing is learning from great mentors. It was great seeing our consultants in action; it was infinitely more engaging than just talking about a paper case over zoom. They made us feel so welcome (and now so bad that we’ve been pulled out again!). In general, our residents were committed to making our short stays as high-yield and non-toxic as possible.
I appreciated this strong culture of mentorship and learning while we rotated in the neurology department. Due to personal reasons, I wasn’t able to really appreciate that week –we were also pulled out as a cluster because some residents in the medicine department tested positive, putting all of us at risk– but I did appreciate one night when the residents and consultants celebrated the graduation of one senior from the program. (We were also treated to free food, aka something I definitely missed over a year of only online conferences and zoom grand rounds).
Rotating during internship felt different from rotating in clerkship. Now I have more confidence. I was relaxed enough to consider perspectives I was too stressed or anxious to see during clerkship. The hospital became more friendly. I saw with more depth the roles of the nursing team, the nutrition department, the pharmacy, and so on. I could talk more easily with residents. I realized they were only a year or two ahead of me –though they have worked through a pandemic, so mad respect there.
The Medical City feels like home. Even though I’ve only spent probably half my clerkship there and only one month this internship, our stay felt like a lifetime. Its halls and cafes and gardens and staff will always carry something familiar to me, no matter where I end up training and practicing.
Thank you for the opportunity to learn. I’ll even thank you for those bloody exit exams.
.

.

.

.

.
Meanwhile, in the community
Let me start off by saying this is the best rotation ever. No bias, except I am considering a career as a family physician in the future…
The pandemic meant drastic adjustments to the family and community medicine program. I was not looking forward to it. Fortunately, our ASMPH faculty stepped up to the challenge and designed a safe yet responsive alternative. In partnership with Healthway Family Clinic, previously FamilyDOC, ASMPH provided an opportunity for interns to have hands-on experience as the “first touch” of many patients in the community.
What’s Healthway Family Clinic? Read more here.
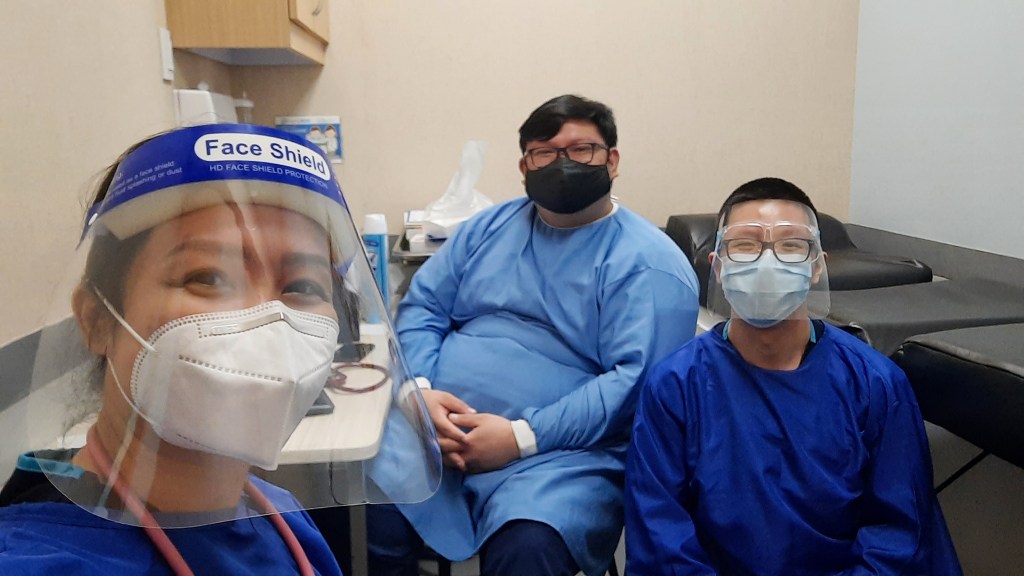
For the entire four weeks of FCHM, two interns are assigned to rotate in a particular branch of Healthway Family Clinic. We start by shadowing the Family Medicine consultant or resident (sometimes it’s a general practitioner on deck) to get a feel of the flow of patient care. After a day or two, we had the privilege of already leading the interview, physical examination, prescription writing, and patient education. Basically, for most of the cases, we functioned as the main doctor in the eyes of our patients (all under supervision, of course).
This experience has cemented my desire to work in the fields of primary care and public health. Somehow. In any capacity.

.
First: Primary care, specifically family and community medicine, provides an unparalleled breadth of cases. In our short two weeks of rotation, I’ve seen kids, gynecologic patients, adults with lifestyle diseases, and even surgical cases, such as minor burns and abscesses for incision and drainage (we didn’t have the facilities to perform minor surgeries onsite, unfortunately).
I value everything I’ve learned medical school, without preference towards one subject or the other. Right now, I just can’t imagine a life where I won’t see a pediatric patient, or a life where I won’t have the privilege of managing minor surgical cases. I still like suturing lacerations; just don’t ask me to stand for 16-hour procedures in the OR. The hyper-specialized life is still not for me.
Second: Ever since I met a family medicine resident in the non-urgent section of the ER, I’ve been on a roll interviewing doctors about the quality of life in their respective residency program. And the quality of life in a family medicine program is almost incomparable. In the TMC program, for example, it’s a 50-hour work week with Sundays off and protected time for didactics and conferences. In the FamilyDoc (now Healthway?) program, it’s mostly just clinic hours with no 24-hour duties and with Sundays off as well.
I can actually have a life. I can study and conduct research and workout and cook and still see a good number of patients everyday. But I am heavily considering training in a public hospital, and for obvious reasons, that’s going to be more toxic and less forgiving. I’m still willing to bet that FM in a public hospital will have better pay and more human conditions than most other residency programs in the country. A part of me might also just train abroad. Who knows.
I can be home by 5:30 PM.

.
Third: Despite the short amount of time, I was able to see glimpses of the ideal primary care and referral network system. On our second week, we were able to see patients coming in for followup from the week prior. It was easy to continue building rapport. I think our patients were also immediately more comfortable the moment they saw our familiar faces. I could see how continued rapport and relationship building can make it easier to ensure not just the individual health of patients, but the health of their family, loved ones, and community.
We had a patient who had to go to another diagnostic center for a service not offered in Healthway Family Clinic. This same patient also had to seek consult with a specialist, so part of the job was looking for suitable consultants for referral. A part of me was concerned that our patient would be lost-to-follow-up –maybe they’d stick to the specialist and never come back to the primary care physician. But they did come back, and they even sent gifts to the clinic!
Because of the trust built over the course of several consults, and the feeling of greater understanding, our patient felt more comfortable with their FM physician. It was up to us to translate the different diagnostics and therapeutics, and to put the specialist’s plans to perspective. Primary care is an answer to the fragmentation of care that happens as a result of multiple specialists treating the same patient without communicating with each other.
As our consultant said, being a family medicine physician also means being a coordinator of care between different specialties. I think that while specialists can be experts at managing a particular system or disease process, they aren’t as equipped to manage everything else. FM physicians can even do marriage counseling! That’s the value of having a generalist on board.
.
Fourth: Wherever I end up practicing, I know that I’ll always champion patient education and the biopsychosocial model. In the family medicine consult, the effort is always worth it.
In the internal medicine outpatient department of Ospital ng Makati, we only had 15 minutes with each patient at most; there was always a long line. Because of this rush to get to the next patient, there’s never any time to unpack whatever barriers face a patient. The same goes with doing rounds in the hospital; you’re in and out of the room in five minutes or less. Back then, an unhappy part of me would think that this or that patient is likely going to be non-compliant to medications, or lost to follow up once discharged. There wasn’t anything I could do about it.
In the family medicine practice, patient education and holistic care are essential. While there will also always be a next patient, somehow FM practitioners can squeeze in an hour of patient care into a shorter amount of time. There’s dedication to not just the medical problem, but the socioeconomic factors that play into it. We even screened several patients for mental health issues.
Fifth: The rotation provided an opportunity for me to shake off the rust from my MBA know-how. How can we best deliver service to patients? I’ve been a long-time believer in one-stop shops for health, such as Healthway Family Clinic. I’ve been similarly impressed by some well-funded barangay health centers I’ve visited (the ones with Gene Xpert, or HIV testing/counselling, or PRC partnerships etc). It’s important to make healthcare as convenient and accessible as possible to our patients, especially those in the lower economic strata.
When FamilyDOC first launched in 2015 under AC Health, it marketed itself as a community-based 3-in-1 center with consultation services, diagnostics, and a pharmacy –basically, all you need for preventive and primary care. I was really impressed by the idea. Though I wasn’t quite sold on their fledgling FM residency program just yet, I was excited by their expansion and diversification elsewhere.
The past two weeks gave me more insight on how this type of center plays out in real life. A lot of the problems in execution boil down to operational roadblocks and poor internal analysis at the management level.

.
With all these great experiences and promising learning moments, I can only feel a resurgence of hate towards the government for continuously failing to contain this pandemic. I admit that I have seen individuals fail to wear masks outdoors (specifically in public markets), and I personally know people who’ve gone on non-essential travel and “errands”. But there is only so much individual action can do; it’s still really up to the government to provide the infrastructure needed to combat the spread and to prevent the surge in cases.
So what do we have? Donated vaccines, lack of transparency in the rollout, a lot of question marks over where our billions in national debt went… And a bunch of family medicine interns now stuck with an online course on Medical Certification of Cause of Death. I appreciate this learning module. But I would have liked doing this along with clinic exposure even more.

.
One pandemic and twelve months ago
One year prior, patient* noted episodes of anxiety, with loss of productivity and changes in behavior, associated with occasional headaches and impaired attention, recurrent, aggravated by radical shifts in routine due to a nationwide lockdown with no other collective health protocols in place. In the interim, barely anything changed…
It feels like we’re back to square one. Maybe even square zero, if it weren’t for the donated vaccines. Hospitals are being converted back into referral centers. Wards and beds are being filled to capacity. The interns and clerks have been pulled out of the hospital. Even the Taal Volcano is back on higher alert.
And in the interim that was March 2020 to March 2021, we’ve lived lifetimes and wrestled with regimes and grown backwards and forwards and upwards. But somehow we’re still here.
Read here: My 2020 in art.
I hope my next update will bear happier news. (Though I do have a couple of poetry and art posts lined up.)

.
It was March 11 2020. Faye and I were duty clerks rotating in orthopedics, chatting about plans for lunch in between shadowing our respective residents. Word started going around that, thanks to the rising number of cases in the hospital and in the metro, clerks would have to be pulled out from rotation. As a clerk assigned to the floors, I even rejoiced when the memo was released. I thought it would be a much-needed break. (Faye at the ER was less ready to go).
The memo released by our dean began, “due to the onslaught of rapid transmission of COVID19 among healthcare personnel, all Year Level 8 Clerks in all rotation hospitals are hereby ordered to be pulled out of their clinical rotations effective immediately, except clerks in community rotations.” Sounds familiar.
When we both got home, we immediately made plans for dinner at a Japanese restaurant in Megamall. Neither of us knew that was the last time we’d go on duty together, and even the last time we’d see each other for close to ten months. Dramatic? Yes. Depressing? Also yes.
It’s March 11 2021. And we’re still here.
.
Until next time!
For similar posts, check out my medical school tag.
*Literally the minute I posted this, I found out that we’ll be back for face-to-face rotations in the community next Monday. This world is so volatile and ever-changing. However, hospital-based rotations still don’t have the green light.

Say something back.