We’re back in the hospital!!! Finally. Though the threat of COVID-19 remains at large, and I won’t be going home anytime soon, nothing beats being back in the thick of actual patient care.
This is a little post on my first two weeks back in the hospital for internship. We spent one week each in the Intensive Care Unit and the Emergency Room. Coincidentally, both of these medical specialties share bouts of high adrenaline situations deciding matters of life and death. But there’s a difference in management goals; it’s either to admit or to discharge in the ER, or to transfer out or to expire in the ICU. Unfortunately.
Week 1: Critical care medicine in the ICU
Critical care medicine is one of the most awe-inspiring subspecialties I have and will ever encounter. Intensivists, or those who care for critically ill patients, have the broad expertise needed to manage multiple organ failure and near-fatal events, to do ultrasound and other advanced diagnostic procedures, to do life-saving bedside surgical interventions, and to comfort the family of those who are truly sick. They come from a background of internal medicine or pediatrics, emergency medicine, or anesthesia.
I was lucky enough to have Dr. Cinco for our first week back in the hospital; he was actually the preceptor of one of the last online synchronous discussions I attended via zoom before the return to hospital duty. Like many other ASMPH professors, he’s dedicated to evidence-based medicine and also to the necessity of humor, somehow. It was comforting to see such a great teacher show enthusiasm for the return of interns (and the eventual return of clerks). I do think that teaching is one of the best ways to continue learning and also one of life’s greatest responsibilities.
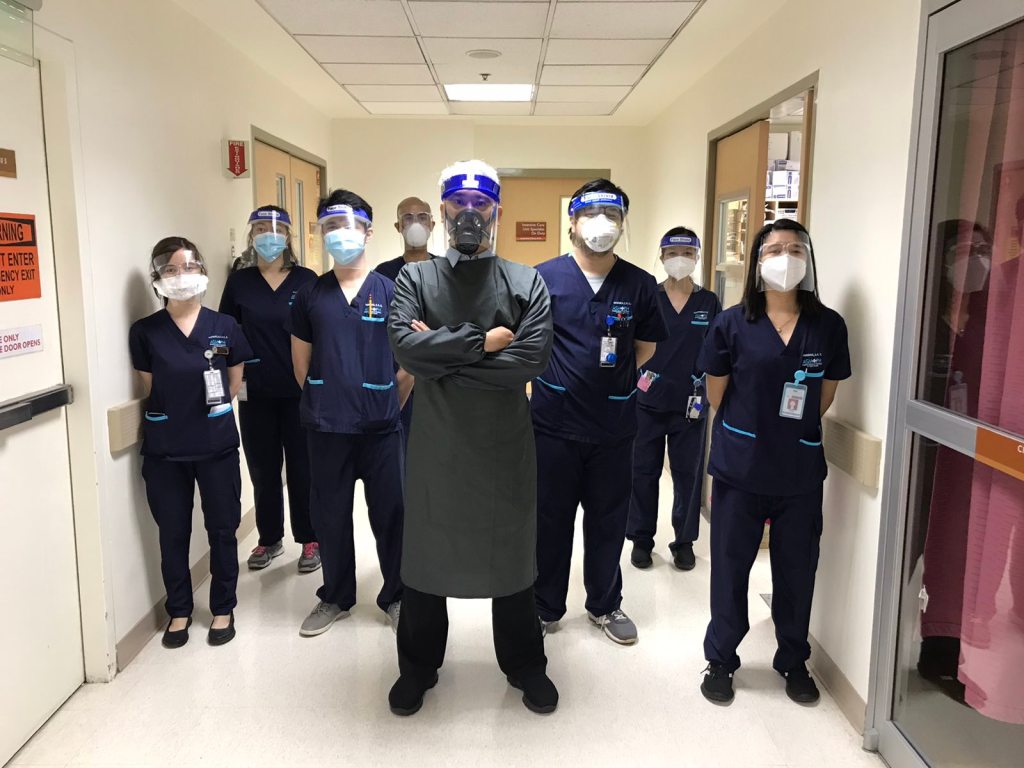
.
Second, the ICU rotation gave us a lot of time to study. It’s almost similar to the ER; there are lulls of activity broken by actual emergencies or urgent situations. But unlike the ER, no one expects change or recovery to happen quickly. Most of our day and night shifts were thus spent monitoring for the response to certain interventions or waiting for results of imaging and other tests. As “precious interns” who can’t be exposed to COVID-19 patients or COVID suspect patients, we had even more leeway.
We were blessed enough to also have friendly and amazing R3s who would take the time to teach us a little something or two. The best teaching moments were still when consultants –the best of the best in TMC– would come to see their patients and update the management plan.
(I do wish there was space for us to actually sit down. My legs were swelling at the end of each shift.)
Week 2: Emergency medicine in the clean ER
A single day in the ER can teach you more than one week of daily didactics. Fact.
On my last day at the ER, which was fairly benign as it was (we only had one emergent patient), I interviewed one allergy patient (their companion triaged earlier had anaphylaxis), a patient with diabetic ketoacidosis, another with acute coronary syndrome (atypical!), and another ACS patient with suspicion for stroke (we called the brain attack team). In the last two hours in the non-urgent station, I was able to squeeze in a patient with abdominal pain, probably surgical, and another with your run-of-the-mill animal bite.
These are all “topics” that would have taken up to a week of theoretical study to exhaust. It only took a day for me to see the presentation, the approach, and the ER-level management. It’s great. I love being back at work.

.
How has the ER changed since the pandemic?
For one thing, there are now two emergency rooms in TMC’s two-hospital system. One is for patients who may have COVID, and another is the clean ER. Our stellar triage nurses are in charge of this division as well. I’ve seen several patients turned away because they had colds or fever. We also need to don protective gear on top of our masks and face shields. Finally, there are definitely less patients (as less people are willing to brave the ER versus a telehealth consult), allowing us to better attend and follow the patients we initially interviewed.
It balances out. The decrease in patient load was matched by a decrease in number of interns and clerks. Our training officers didn’t want us crowding too much in the emergency room. Thus, out of our 7 days nominally in the ER rotation, we actually spent three days assisting the medicine residents assigned to the floor. A nightmare. I hate paperwork. I cannot wait for the new tablet-based EMR system to kick in.
.
Even with the limited number of days, this ER rotation was a lot better than the one I had in clerkship in terms of quality. Because we only had one or two patients per hour on average, it was easier for me to process what was happening and to contribute to discussions on interpretation of diagnostics and on management. It was also a lot easier to build rapport with patients and to practice skills because there’s less pressure to rush to the next patient.
From generalist to specialist to generalist
It’s only a couple of months until our licensure exams, and I’m still fairly set on a future in public health and family medicine. But if I had to choose another specialty, I’d consider Critical Care Medicine, Endocrinology, and Emergency Medicine. In that vague order.
I don’t want to be the kind of consultant who’s super-specialized to the point of forgetting the basic points of general practice. I also don’t want to keep seeing the same set of diseases all the time. Unfortunately, there’s a natural incentive for specialists to stay updated only on the diseases they handle the most; specialists don’t have the time to read up on all the guidelines across different specialties. It’s simply easier to refer a case to someone else for problems outside the usual scope.
Thus: CCM, endocrinology, and EM. To me, these specialties require a generalist’s approach.
Critical care medicine practitioners have to deal with multiple organ systems failing within a single critically ill patient; they also need to mediate multi-disciplinary teams for best patient care. During our stay in the ICU, I appreciated (1) the culture of continuous learning and the drive to read on the latest RCTs regarding interventions, and (2) the strong theoretical foundation on physiology and pathophysiology underlying the interdisciplinary management of disease. You need to know everything. Also the diagnostic and therapeutic bedside procedures were impressive to see.
Next up is endocrinology. Cases are still likely to be diabetes and goiter 90% of the time, especially in the Philippines. However, endocrinological problems tend have strong relationships with a person’s lifestyle, whether as cause or effect. Practitioners of this specialty still have to take a more holistic biopsychosocial approach to health compared to others (in my opinion). Also, from a public health perspective, endocrinology-related diseases are practically second only to cardiopulmonary diseases in terms of preventable morbidities. Also also, I really admire the endocrinologists I know.
Finally, emergency medicine. I almost got sold to it by the EM residents. Not really. No patients to chart day by day, with a schedule that’s more forgiving than the pre-duty-from traditional (or essentially duty-duty-duty) of first-year medical residency. You need to know a little bit of everything, especially the near-fatal and fatal conditions of each system, no matter how rare they are. But at the end of the day, I’m not fit for the high-stress lifestyle of EM. I like taking things on my own pace and talking to people and building relationships. And I also want the time to educate patients and see how their health can be further optimized, not just secured.
(An internist’s life in the hospital, despite the opportunities for follow-up, patient education and disease prevention, ain’t it for me. No thanks!!!)
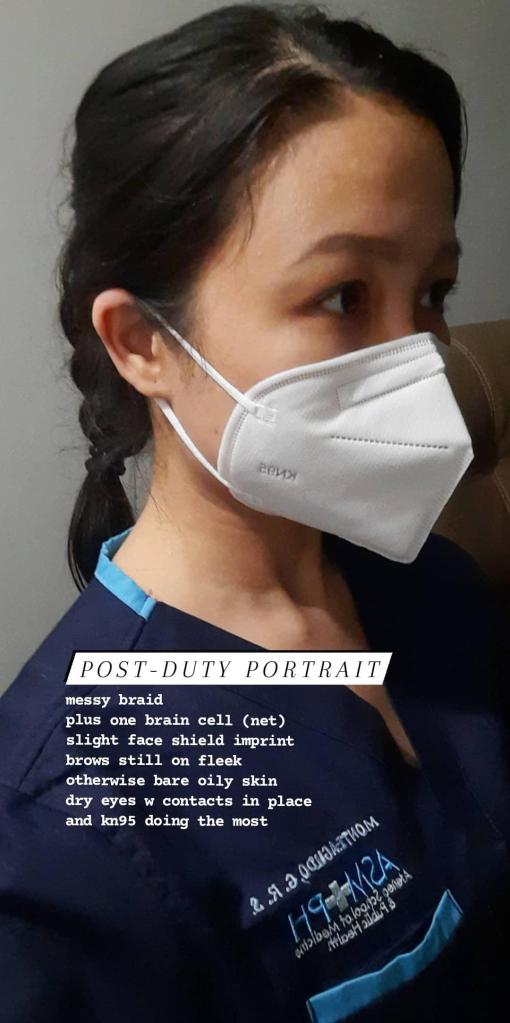
Side note A: Adjusting to daily PPEs

Day 2 (or so): After a quick stop to an optical shop for contact lenses, I was much happier and my ears lighter. I also had several ‘earsavers’ on the way, thanks to pasabuys with friends.
.
Side note B: Back to clerkship
Internal medicine was also my first rotation during clerkship! So these first two weeks were a hit of nostalgia for me. I still had Doc Cinco as the consultant for my ICU week, and even our R3s (third-year residents) in the ICU were the first-year residents we used to follow around back in 2019.

.
I didn’t get a photo this time around, but here’s me back in 2019 with Doc Tony. I can’t believe the R1s that used to stress about admissions and census updates are now seniors ready to graduate from the program. Doc Nicole, who was Faye’s R1, is now chief resident??? Time flies when there’s a pandemic.

.
And here’s a photo of my OG duty group back in the ER! I saw some of the nurses we first met back in 2019 also, like Sir Shimizu, Sir Ray, and Ma’am Kate (but naturally I was always a little too shy or too tired to socialize this week). I did spend more time getting to know the NU nurses this time around –thank you Ma’am Jesse and Daisy and Joy and Sir Daniel (?) 💖
I even saw some of the same family medicine consultants in the NU, and Doc Nica O again in the ER (but not Doc Frances, unfortunately). Doc Irene was now calling the shots. I love that energy.

.
Imagine if I actually went to The Medical City for residency. As if. I’d be having these nostalgia posts every year.
Side note C: Continuity of learning and care
Though I may or may not grouse about the 72-hour work week in the middle of a quarantine, the design of the medical rotation has been excellent for following patients and their course. The ICU patients that I saw during my first week were also there to greet me in 7B, the telemetry unit, when I rotated the floors during my second week. Some of the patients I saw in the ER were also patients that I now see in my week in neurology; most of these were admitted for dizziness or stroke. The finer details are naturally in my personal journal (or in my rapidly fading memories).
With only four weeks to a rotation, this has been a surprisingly great way to understand why different subspecialties and teams do certain interventions and how patients respond also through the spectrum of hospital-based care. Thanks to a more solid theoretical foundation, and the fearlessness that came with surviving OB rotation in QMMC, my perspective now as an intern is leagues away from my old perspective as a clerk.
I’m looking forward to seeing what else I can learn in the next two weeks. Until then!
Say something back.