Status post ophthalmology, psychiatry, neurology and rehabilitation medicine, also known as the six “chill” weeks between Internal Medicine and Obstetrics & Gynecology.
mind, body and soul (and the eye)
There’s something indescribably profound about the human mind. Before I knew anything of actual medical practice, I wanted to be a neurologist. I was that baby doctor who aspired towards the most unknown and unknowable of practices.
I was ensnared by the thought of working with one of the greatest mysteries left on earth –next to the fate of Amelia Earhart and why exactly the Marcoses are still in power. As a medical student, the mysteries are still mysteries, but I at least know a thing or two more about localizing lesions.
The past few weeks have been an exploration of that final human puzzle. We only had a week’s worth of rotation in The Medical City’s Neurology Department, but the other minor rotations bracketing that week felt like extensions of each other –much like how the mind and the brain and our view of the world are all inextricably linked by culture and biology.
So yes, count me very happy to have lived through the past six weeks of ophthalmology, psychiatry, neurology and rehabilitation medicine.

Ophtha: a vision of the ideal consultant life
Of the many tips you’ll hear in medical school, how to choose your residency is a favorite. Is it about what pathologies excite you? The usual work schedule? Or is it about the projected salary?
The consensus says it’s a big mix of everything, but the more important thing is to imagine your life as a consultant (versus choosing your specialization based on the life of the resident, which is guaranteed to be hell in 90% of all possible paths).
Ophthalmology consultants sit right at the top of the ideal list. You’ll likely never be summoned off-schedule to the hospital (there’s only one eye emergency I can think of, and the rest can wait until office hours the next day). You’ll have a blend of medical and surgical challenges to entertain you. You’re unlikely to face death in the operating room. You can go in for some surgeries and earn your family’s yearly grocery allowance within a day or two. The work-life balance is wild.
But then again, it’s not easy getting there. You’ll need millions in equipment to set up a practice. And for some people (like myself), you’ll have to get over the very limited scope. My eyesight is the most precious sense to me, but I still can’t get over focusing on only the eyes for years and years, especially after a decade of systems learning.




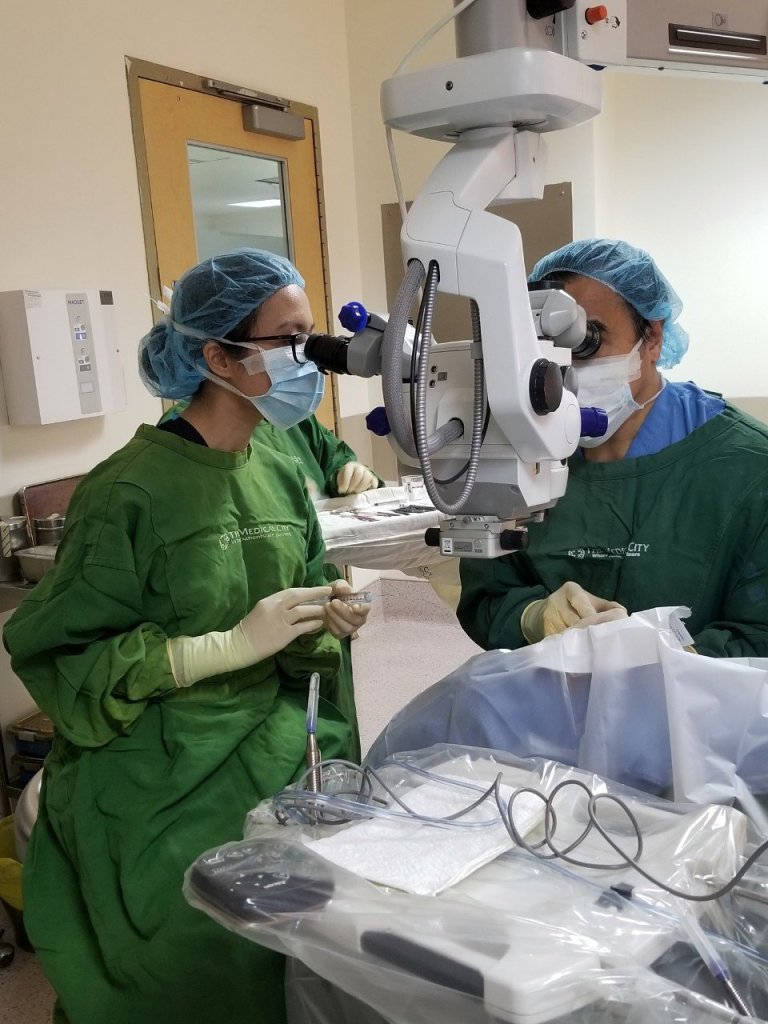
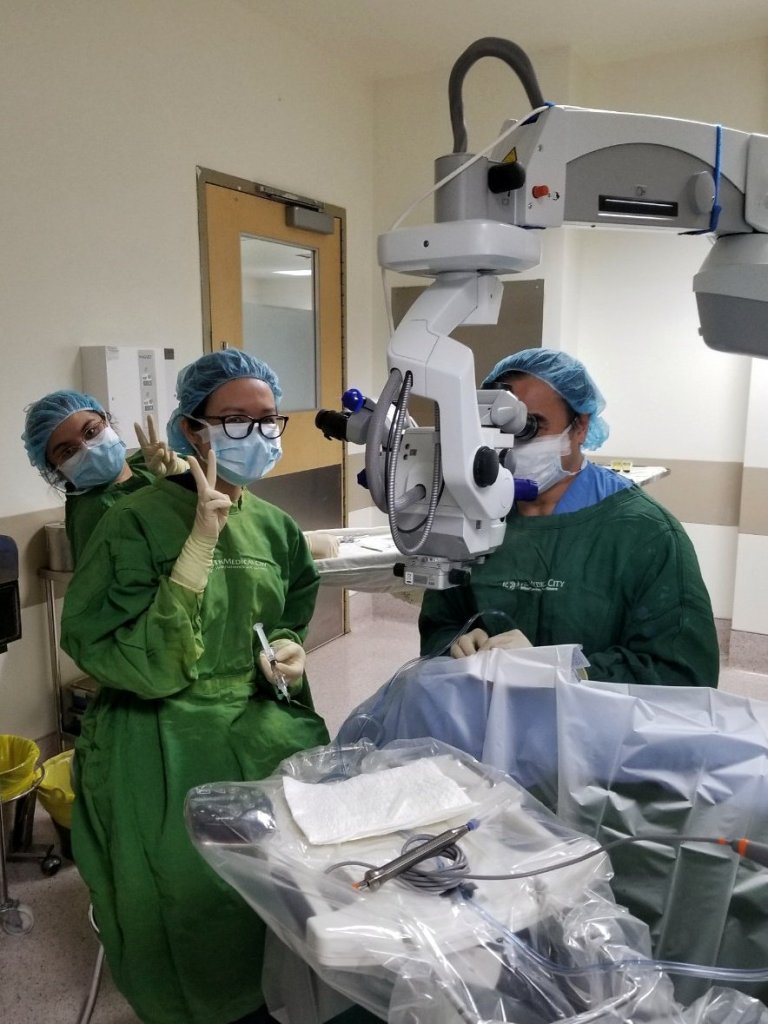

Psych: the plot thickens
As in, the plot is long enough to take 1.5 hours to get rolling. I’m seriously considering psychiatry as my specialization, but I will need to think about whether or not the emotional exhaustion and long interviews are worth it.
I love listening to patients tell their stories, even those whose ramblings seemed too difficult to follow. And I love relaying it to others. As trite as it sounds, I firmly believe that every person is unique and full of depth. But mental illnesses have a way of removing that agency by destroying a person’s insight and functionality.
Sometimes all we need is someone who will listen. Sometimes what we need is directed intervention from a psychiatrist. It’s all valid.
One of the most rewarding parts of psychiatry comes right at the start, at the moment of initiating a conversation. It’s already one step closer towards stopping someone from committing suicide, or towards helping someone gain understanding of themselves. Another thing I found rewarding was the challenge of biopsychosocial formulation –piecing together someone’s disjointed stories to understand their becoming and being. It’s like writing a detective story in reverse.

We spent two weeks in this rotation. One week was spent in Metro Psych Facility, which is a long-term facility for patients with mental illnesses. It also has a facility for those who are recovering from substance use disorder (e.g. alcohol or drug addiction).
The next week was spent in The Medical City’s lower ground floor, which was an unfortunately more gloomy place. We did get to cook chicken cordon bleu with our patients, though!


Neuro: BRAIN ATTACK TEAM
It was my brain that was attacked.
Just kidding. I love neurology (as my incredibly long introduction can attest), and I’m definitely looking at it as a possible career after medical school. But I’m not confident about discussing neural pathways and localization and pathologies yet. There’re just so many things that can go wrong with our nervous system. I’m hoping that academic mastery will come when I actually take the time to study aka a few days before the end-of-year finals.
What I learned from our amazing residents include: how to do a quick but thorough neuro physical exam, how to survive a duty shift filled with never-ending referrals and admissions, and how to make stroke/neuro patients feel comfortable and adjusted to their new status quo.
I will never forget the smiles of patients and their families when they would greet and thank the neuro residents during rounds. They even cracked jokes! Neurology is truly a practice in the saying “to cure sometimes, to relieve often, and to comfort always“.


Rehab: “Thank you po.”
Entering rehab rotation, I was a confused mess (to be fair to myself, I was post-duty status on that first day!). I was there in Philippine Orthopedic Center, wondering why any doctor would choose rehabilitation medicine.
There were many things that disoriented me. First, 90% of rehab patients are referrals from other services. You’re never actually their “main” doctor. Second, there was simply a whole other language to rehab. Their prescription pads don’t contain medications or the usual battery of diagnostics. It’s a list of physical modalities and exercise for the receiving therapist.
But! And there’s always a but—-
All of the patients are so damn thankful. It’s because rehab isn’t there to directly treat or cure a disease. It’s a specialty that put the premium on care and long-term progress. It’s the aftercare all patients should get.
So when a patient says “thank you” for letting us move their limbs around for a tiny bit of improvement, it feels momentous and really special. Quality of life and functional activities of daily living over everything else.
(Rehabilitation medicine is also in some ways a more direct application of basic medical concepts, especially anatomy and physiology. It really takes you back to the early days.)
Finally, one of the BEST things about rehabilitation medicine that I can say I’ve never seen in any of my other rotations is the multidisciplinary approach. The full health care team is on board. It’s not just one specialty to another, like you’d assume it would be limited to the orthopedic surgeon and the rehabilitation specialist.
At least in POC, the rehab grand rounds are composed of the rehab doctors, the attending physical therapist, occupational therapist, nurse, psychologist, and even social worker. All of these allied professionals have a direct role in the improvement of a patient’s quality of life, and I really appreciated seeing that in action.

The most stressful chill weeks of my life
On the first few days of our first week in ophtha in Quirino Memorial Medical Center, I felt depressed and anxious and even ashamed of how rusty my skills were. On the 2nd week of ophtha, an otherwise wonderful rotation was punctuated by news of my godmother’s passing.
The first week of psychiatry was a scheduling mess, on top of my high stress as our group’s rotation leader, and the next week made us feel like trespassers instead of team member-learners. (It was during the department’s accreditation week).
The neurology rotation was inspired, but full of brief high stress moments interspersed with long stretches of nothing, and rehabilitation week was literally hot and almost alien in its language, at least for the first few days.
And yet the last 6 weeks gave me insight to the kind of resident and consultant I wanted to become. I learned baby steps of the interpersonal and technical skills I wanted to embody in the future, the brand of professionalism I want to endorse, and the level of competency I want to inspire in future doctors as well. Basically, it was 42 straight days of looking at this-or-that doctor and thinking #GOALS.
OUTTAKES
No rest for the wicked, except for fun foodie side trips in Banawe and shopping in Rockwell. I also got a chance to wrap up Finman, visit Nagcarlan with my family, have dinner with Maryan, and appreciate some random art.













That’s all there is. :)
See you next time for a recap of ENT/OB, unless something more exciting comes up in the mean time (AKA WATCHING SWEENEY TODD AND GOT7 #KEEPSPINNING).
P.S. Publishing this long blog post while at the RR??? Thankfully all of our patients have stable (or stabilizing) vital signs.
Say something back.